AI-Powered Triage and Clinical Decision-Making Support (CDS): KATE AI
A growing share of younger, less tenured nurses are entering the workforce. As one executive from Adventist Health noted, "Across the country, we are seeing decreasing levels of experience in our frontline nurses while patient complexity increases." KATE AI's triage and acuity support tool addresses this challenge by acting as an extra set of eyes, enhancing nurses' clinical judgment and ensuring that no critical details are missed. By improving patient acuity prioritization, KATE AI enables earlier interventions and provides both executives and nurses with greater confidence in care delivery.
Adventist Health's implementation of KATE AI revealed three critical success factors for other organizations to emulate: 1) schedule training outside busy clinical hours rather than during shifts, 2) position AI-enabled CDS as a supportive partner rather than an error-detection tool, and 3) incorporate real-time feedback mechanisms that preserve clinical autonomy while enabling continuous improvement. Successful AI-enabled CDS adoption depends as much on thoughtful change management as on the technology itself.
Adventist Health profile
Location: Headquarters: Roseville, CA
Facilities: 440 sites-of-care
Health system type: Nonprofit
Timeframe: 2019 - present
Program goal: Enhance emergency department triage accuracy and efficiency while supporting nursing staff confidence and improving early detection of time-sensitive conditions
Scaling status: Piloted in 3 emergency departments in Southern California, currently scaling system-wide in 22 Emergency Departments
Key metrics
Provides alerts within 1-8 seconds after a triage form is submitted
40% improvement in sepsis detection rate scores
96% of nurses triaging 10 or more patients engaged with at least one KATE AI engagement. In 34.5% of cases, nurses took action after receiving a KATE notification - adjusting the ESI level, vitals, or reason for visit narrative - demonstrating strong trust in and engagement with the tool.
The solution
KATE AI assists with triage support and validates acuities for patients with all types of conditions. KATE alerts triage nurses within 1-8 seconds after a triage report is submitted, notifying clinicians of high-risk conditions the patient may have based solely on existing EMR documentation (e.g., sepsis, stroke, heart attack, preeclampsia, etc.).
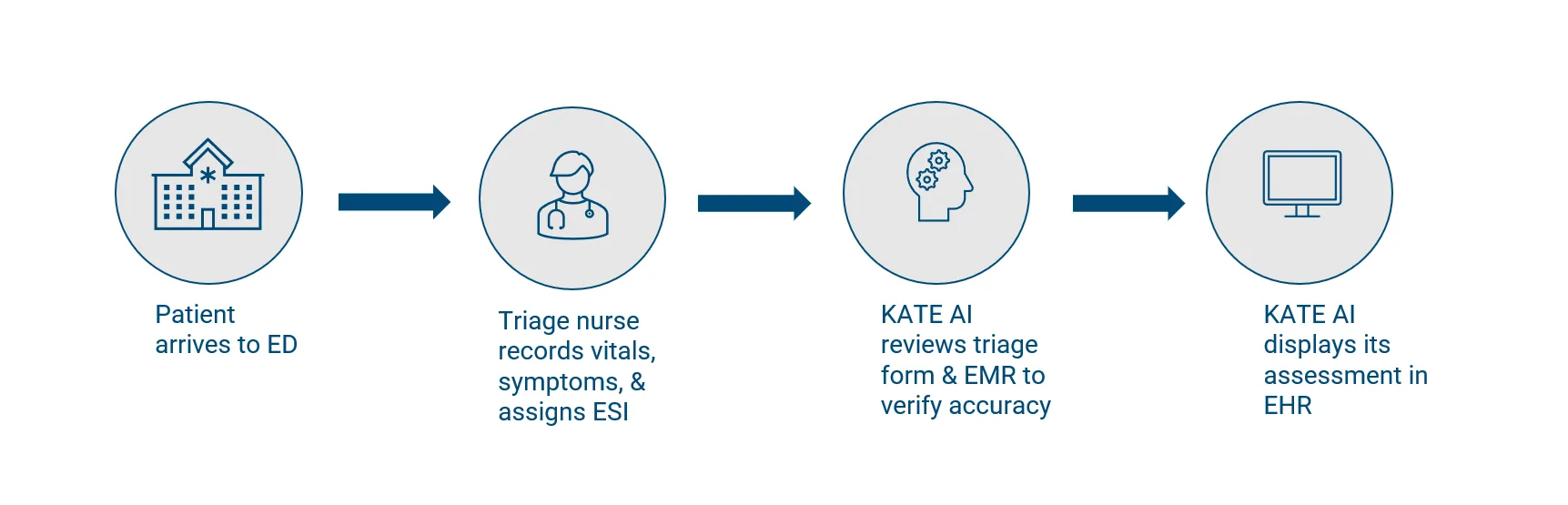
How it works
Step 1: Triage nurses document vital signs, symptoms, and other relevant information into the triage form and assign an Emergency Severity Index (ESI) based on their assessment and clinical expertise.
Step 2: Once the nurse submits a patient’s triage form, KATE AI scans the patient’s medical record and triage form, uses AI risk models to evaluate the assigned acuity level, and identifies any missed high-risk conditions or factors.
Step 3: Within 1-8 seconds of triage form submission, KATE AI appears in the EHR only when a high-risk alert is triggered – such as sepsis or preeclampsia, or when KATE disagrees with the nurse’s assigned acuity level. In these cases, KATE AI verifies the Emergency Severity Index (ESI) assignment and alerts clinicians to potential critical conditions. For approximately 75% of its recommendations, KATE AI provides a rationale explaining its clinical reasoning, with ongoing development to expand this transparency feature.
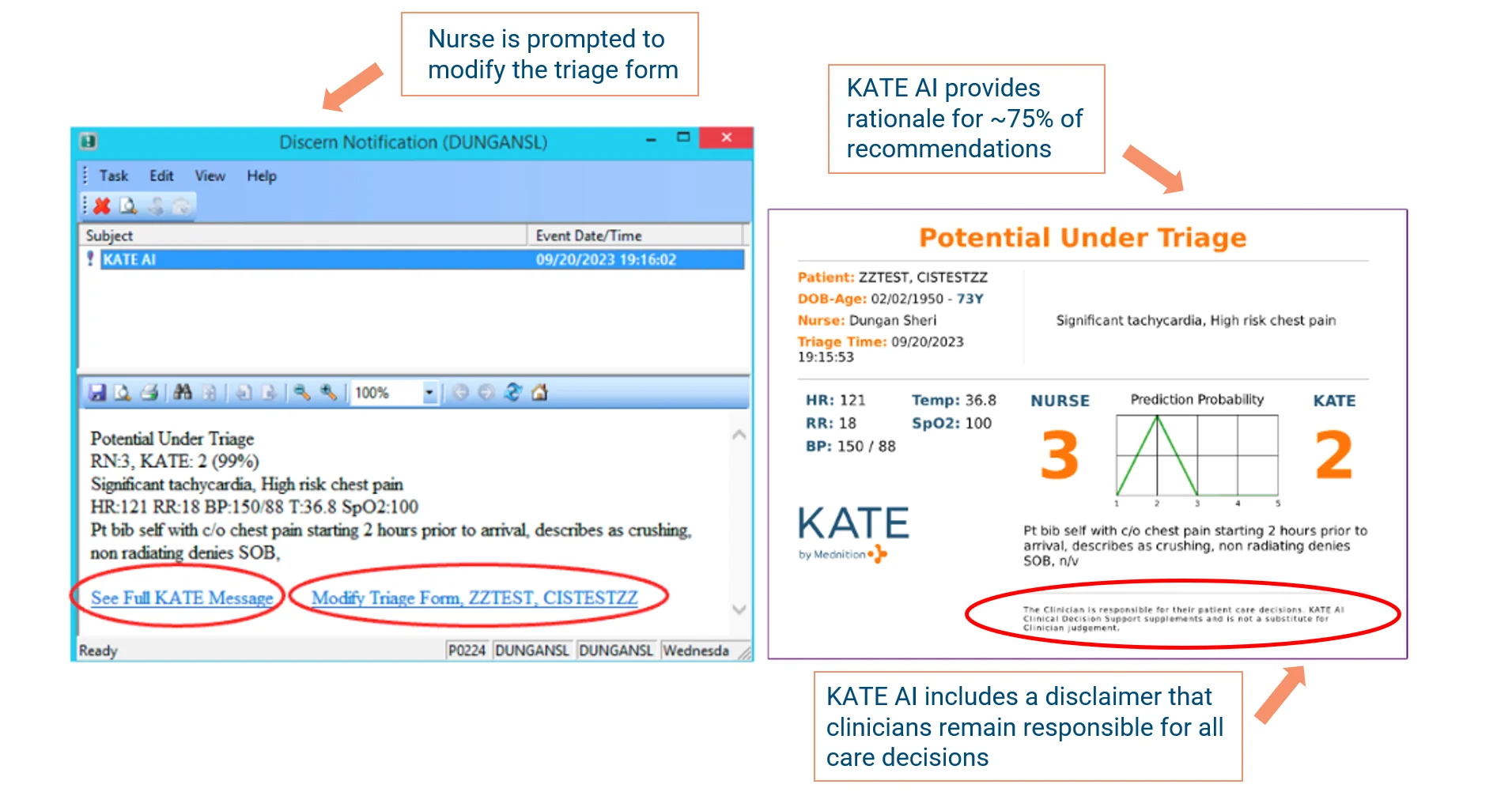
Step 4: If nurses do not agree with patient ESI or critical condition alert, they can provide feedback directly to Mednition through a feedback box in the patient's chart.
Lessons for other health systems
1. Prioritize structured change management by scheduling training outside active clinical hours and clearly communicating the how, what, and why: Adventist Health found that live technical training for triage nurses during busy, high-stress ER shifts was ineffective. In retrospect, they believe holding online sessions outside of peak hours would have ensured staff could fully engage, ask questions, and build confidence before implementation.
2. Position a clinical decision-support tool as just that – a tool that supports clinicians' decisions, not one that tells them what they did wrong: Adventist HealthCare found that framing dramatically affects nurse adoption. As their ED Clinical Practice Specialist explained: "We don't want nurses thinking, 'Great, another alert. What did I do wrong, KATE?' It's not about doing something wrong – it's a decision support tool that's there to help." By positioning KATE AI as a collaborative partner rather than an auditor, they achieved 96% nurse engagement. When KATE AI explains its clinical reasoning (in ~75% of cases), it displays a disclaimer that clinicians remain responsible for final care decisions.
3. When adopting a clinical decision-support tool, ensure clinicians can give immediate feedback when they disagree with the output for real-time iteration: Adventist Health worked with Mednition to build a feedback capability into KATE AI – a feedback box in the patient's chart allows nurses to report disagreements or ask questions about the tool's recommendations. The Mednition team analyzes this feedback and typically responds within 7 to 10 days directly to clinicians. Depending on the nature of the feedback, they may follow up with nurse education, or update KATE’s model to reflect site-specific language or clinical context. For example, if an acronym or phrase has a different meaning at a particular hospital, KATE can be locally retrained. This process helps identify when the AI makes errors, enabling continuous improvement while ensuring clinicians retain final decision-making authority.
